The Ultimate Guide To Fertility Testing, From A Reproductive Endocrinologist
Sometimes, even when you’re tracking your cycle and timing intercourse, you may not be able to conceive. Six months go by, maybe a year, maybe more, and nothing. You feel like you’ve tried everything—and you’ve definitely tried a lot. I know how frustrating this can be. So many patients come to my office feeling this way. I’ve felt this way. Infertility can be a debilitating experience. It’s also a very common one.
Infertility is defined as the inability to get pregnant after twelve months of regular, unprotected intercourse. It is something nobody is prepared to experience. But the hardest experience for me is seeing patients in my office later than I should. It’s extremely important to know how long is too long and to learn to identify the signs that you should get a fertility evaluation sooner rather than later.
Navigating infertility
When my patient Ruby came to see me, she was thirty-two, healthy, and her cycles were regular, occurring every twenty-eight to twenty-nine days. She could easily detect ovulation with CMM and a temperature shift, and she and her husband had no problem having intercourse. But when she’d seen her doctor, she was told they needed to be trying to conceive for a year before having fertility testing. So, they’d kept trying. After another six months, Ruby still wasn’t pregnant.
After a full year of tracking and trying, Ruby went back to her doctor and fertility testing was ordered. Her partner had a semen analysis as part of their testing, and when the results returned, they were shocked to find out he had no sperm. Ruby couldn’t believe they had been trying for so long, putting so much effort into tracking and timing, and the entire time there was zero chance of pregnancy.
Unbeknownst to him, Ruby’s husband had a birth defect that resulted in him not having a vas deferens, important in sperm transport from the testes in ejaculation. It is like being born with a vasectomy–permanent birth control that he never knew he had! They would have to do IVF with a surgical procedure for her husband if they wanted to conceive.
Here is the truth: You can call a fertility clinic and get an appointment with a fertility doctor anytime. You do not have to wait for anyone to tell you that you need to schedule an appointment. I don’t need your doctor to send a referral. We will get your medical records if you have had any testing completed. Don’t let time make a decision for you.
My goal as a fertility doctor is to make the infertility journey less scary. I went into this field because I love it—understanding the hormone puzzle and forming deep connections with my patients make being a fertility doctor truly special. But this job is not all rainbows and sunshine. It is hard, full of emotions and tears, and there are days I am reminded of just how unfair life can be.
My own experience with infertility has forever changed how I approach patients. I didn’t want to admit we had infertility, and I delayed getting testing or seeing a doctor myself. I wanted the problem to fix itself so I could move on to that next chapter of life. Seeing a doctor felt like an acknowledgment of my failure. What if nothing worked? My own denial held me back. If you are there, know that I have been there too.
The unknown of infertility is often the scariest part. We can’t always control the outcome, no matter what we do. This means it is important to focus on what you can control:
- The way you understand your body
- That you know what you are doing and why
- That you are confident in the plan
We can’t rewind the clock. I wish we could. What we can do is know we made the best decision we could with the data we had. No matter how this journey ends, we can leave with the knowledge that we would not have done anything differently.
Fertility testing and evaluation
You should not be forced to wait any amount of time or prove you have infertility in order to have fertility testing. My dream is that fertility becomes proactive, with early testing and preventative measures emphasized. You should not have to fail first before seeking care. If your periods are irregular, extremely painful, or you have difficulty with intercourse, you should seek evaluation now. If you feel like something is wrong, trust your gut.
Over 70 percent of couples who will conceive do so in the first six months of trying. Although it is fine to wait until you hit that one-year mark of trying to get a fertility evaluation, it is also perfectly reasonable to do so before then. Due to the impact of age on fertility, women who are thirty-five or older should get an evaluation after six months of trying.
Your initial fertility consultation is nothing to be nervous about. Your doctor will start by reviewing your medical history. Be prepared to walk through your goals, history, and prior testing or treatment. The majority of the first consultation will be educational, and a fertility doctor will discuss the standard evaluation and appropriate next steps. Preconception testing (reviewed in chapter 6) will typically be ordered at this time if it wasn’t completed prior to your fertility consult.
Standard fertility testing includes:
- Evaluation of ovulation
- Ovarian reserve testing
- Anatomic evaluation
- Semen analysis
Evaluation of ovulation
The best way to confirm ovulation is a great menstrual history. Regular, predictable cycles with a normal luteal phase indicate no further testing is needed. If you have cycle tracking data with any inconsistencies, please be sure to let your doctor know. Below are potential tests that may be ordered for irregular or absent cycles.
Evaluation of ovulation
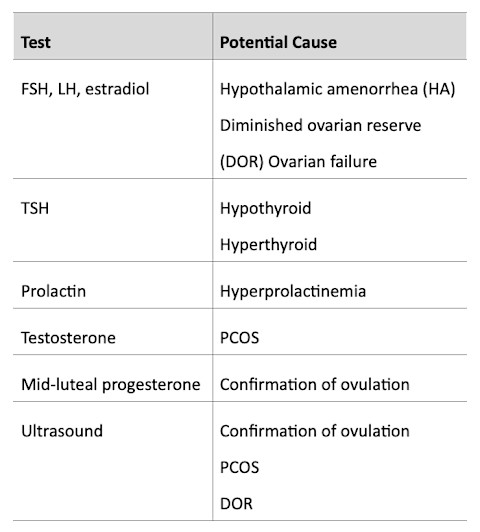
Ovarian reserve testing
Ovarian reserve testing is an approximation of how many eggs you have remaining. Individual levels should be reviewed based on age. All patients getting a fertility evaluation should have their ovarian reserve tested, as it can significantly impact treatment plans.
Evaluation of ovarian reserve
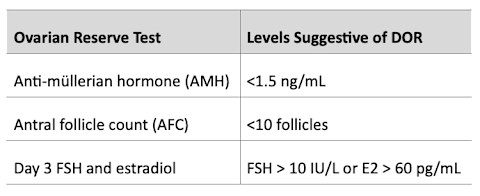
Anatomic evaluation
A typical anatomy evaluation begins with a transvaginal ultrasound (TVUS) to evaluate the ovaries and the uterus. Additional tests will be required to evaluate the inside of the uterine cavity and the fallopian tubes, often a hysterosalpingogram (HSG), known as an X-ray dye test, or an ultrasound-based evaluation, known as sono-hysterosalpingography (sono-HSG). Below are other possible imaging options.
Imaging options for anatomic evaluation
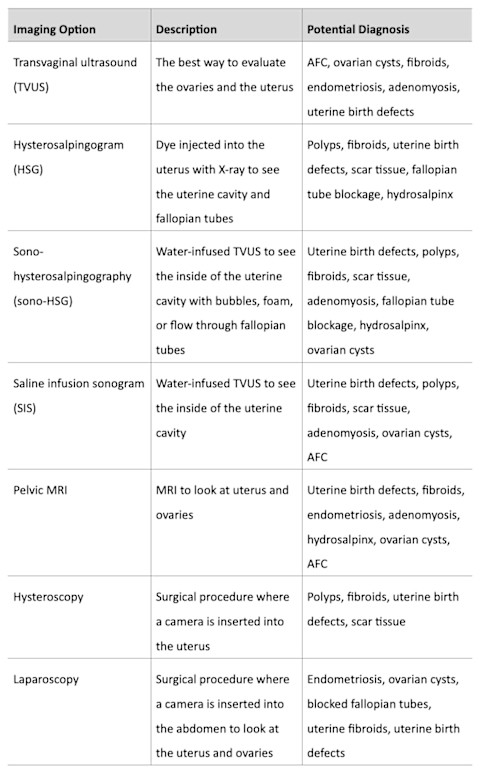
Semen analysis
A semen analysis is an evaluation of sperm parameters, including volume, pH, concentration, motility, and morphology (shape). For a semen analysis, we want two to three days of abstinence prior to sample collection. Longer abstinence intervals are not recommended unless specifically requested by your clinic, as this can increase the amount of debris and dead sperm. If the semen analysis is normal, no further testing is usually needed. Abnormal results may necessitate repeat semen analysis, hormone testing, genetic evaluation, or urology referral, pending the specific abnormality.
It’s important to note that the low end of normal and the ideal sperm parameters for conception are different. If all the sperm parameters are barely above the minimal threshold for normal, the semen analysis may be called “normal” but fertility will be reduced.
Semen analysis parameters
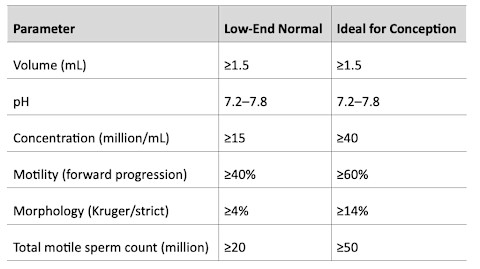
One way to evaluate the reproductive potential of a semen analysis is to calculate the total number of moving sperm in the sample, called the total motile sperm (TMS). The TMS is calculated by the following formula: volume (mL) × concentration (million/mL) × motility (%). A TMS count above fifty million moving sperm is ideal for conception.
Sperm concentration is a sign of proper communication between the brain and testes and represents hormonal function. Motility and morphology are factors that may be influenced by the structure of the testes themselves or the environment. If your partner has an inability to achieve or maintain an erection or failure to ejaculate, that information needs to be disclosed so a bigger evaluation can be completed.
The above has been excerpted from The Fertility Formula: Take Control of Your Reproductive Future (Natalie Crawford Free; Penguin Life, 2026).
